Wounds & Diabetic foot ulcers
Diabetic foot ulcers (DFUs) are serious, open sores occurring in approximately 15% of diabetes patients, often caused by neuropathy, poor circulation (PAD), and, in 85% of cases, leading to lower-extremity amputations. These wounds, typically on the sole of the foot, require immediate medical attention for infection management, specialized off-loading, and proper wound care to prevent severe complications.
Key Aspects of Diabetic Foot Ulcers
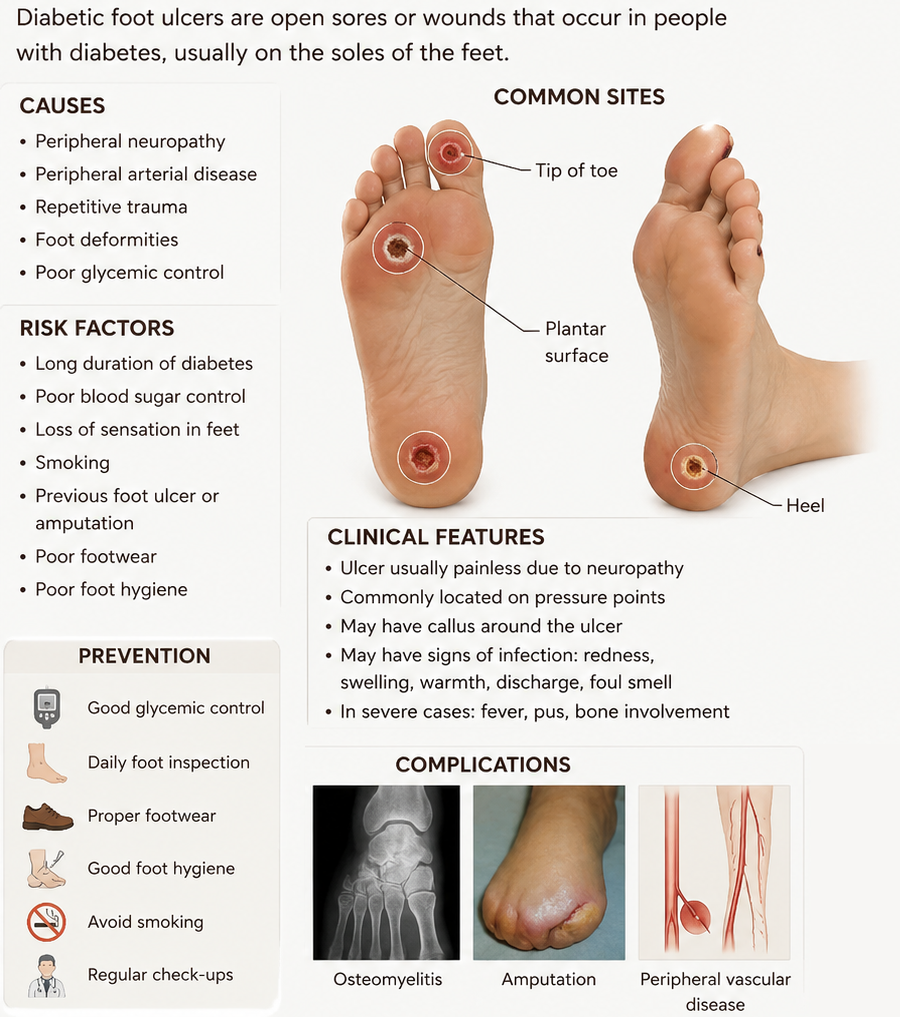
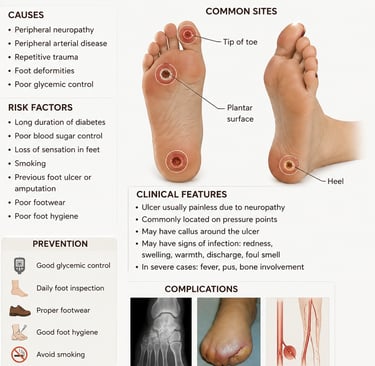
Causes: The primary causes are peripheral neuropathy (loss of feeling) and peripheral artery disease (poor blood flow). Neuropathy prevents patients from feeling injuries, while PAD reduces healing ability.
Common Locations: Most often appear on the plantar surface (bottom) of the foot, particularly on pressure points like the heel or metatarsal heads.
Risk Factors: Longer duration of diabetes, age, tobacco use, obesity, and poor blood sugar control.
Symptoms: Redness, swelling, foul odor, drainage, or callous formation, often appearing as a punched-out, deep ulcer.
Management and Treatment
Off-loading: Essential for healing, this involves taking pressure off the wound using specialized shoes, crutches, wheelchairs, or total contact casting.
Wound Care: Wounds should be kept clean, covered, and moist, rather than left open to air, which is harmful.
Infection Control: About 50% of ulcers become infected, requiring antibiotics or, in some cases, hospitalization.
Prevention: Daily self-checks for sores, blisters, or calluses, along with good diabetes management.
When to Seek Immediate Care
Any sign of infection—such as severe redness, swelling, warmth, or pus—requires immediate consultation with a podiatrist, as these infections can quickly escalate and threaten the limb.
Contact
Reach out for expert foot and ankle care
Call Us
248-471-3312
© 2026. All rights reserved.